The persistent pain of a migraine is more than a headache. This neurological disease can disable a person, and traditional treatments fail for many. A novel approach has emerged from an unexpected source: ketamine therapy.
Originally an anesthetic, ketamine infusion therapy now offers a distinct path for relief where other options have ended. Its use represents a shift in migraine management, focused on complex cases and recalibrating the brain’s pain response. This therapy is not a first-line treatment but a specialized tool for specific circumstances. It marks a move toward personalized, neuro-focused solutions in neurology.
Ketamine Targets the Brain’s Pain Pathways
Migraine pain involves complex brain networks and chemical messengers. Ketamine interacts primarily with the glutamate system, a key driver of brain signaling. It blocks a specific receptor, the NMDA receptor, which is active in pain transmission and central sensitization. This blockade can disrupt the cycle of chronic pain that entrenches migraine disorders. The effect is a temporary reset of the brain’s pain-processing centers. This mechanism differs from conventional medications that target inflammation or blood vessels. Ketamine addresses the neural hyperactivity that defines migraine pathophysiology.
The Protocol Involves Supervised Infusion Sessions
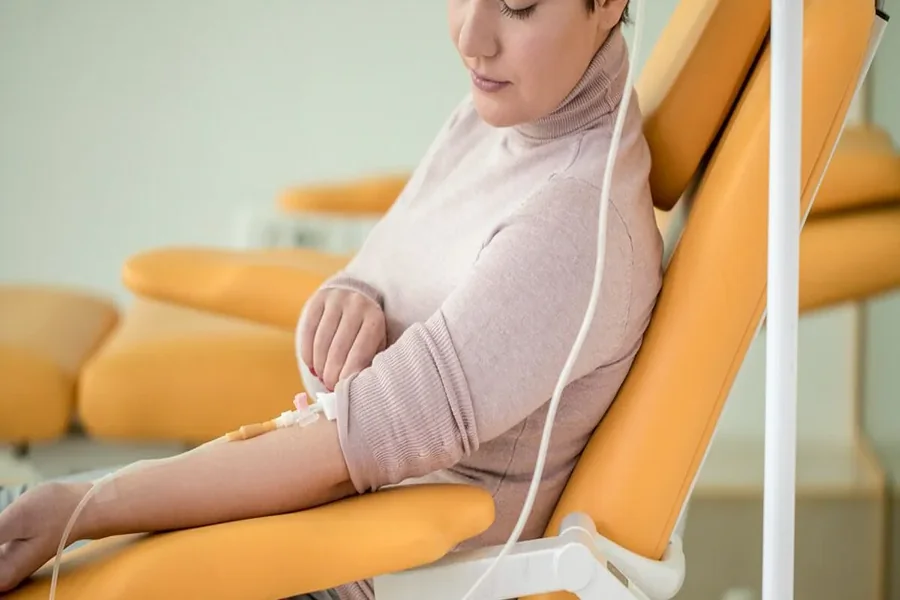
Ketamine for migraine is administered intravenously in a clinical setting. A patient receives a low-dose infusion over several hours. Medical staff monitor vital signs and side effects throughout the session. A treatment course typically includes multiple infusions scheduled across weeks. This controlled environment ensures safety, as the dissociative effects are closely managed. The goal is to achieve a cumulative therapeutic effect that outlasts the treatment period. Each protocol is tailored to the individual’s response and tolerance.
Treatment Serves Specific Patient Populations
This therapy is reserved for particular migraine diagnoses. Candidates include those with refractory chronic migraine who did not respond to standard treatments. It also shows promise for individuals with status migrainosus, a persistent attack that lasts over 72 hours. Some patients with New Daily Persistent Headache may also find benefit. The treatment is considered for cases where the disability is severe, and alternatives are exhausted. Patient selection is a critical step conducted by a specialist. It is a targeted intervention for complex neurological disease.
Patients Report a Reduction in Pain Intensity
Clinical outcomes focus on measurable pain relief and functional improvement. Many patients experience a significant decrease in headache days per month. The severity of breakthrough pain can also diminish. Some achieve a complete cessation of a prolonged migraine attack. This relief can restore a person’s ability to perform daily tasks. The treatment effect can persist for weeks or months after a series. These results provide a window of improved function for comprehensive care.
Integration Demands a Comprehensive Care Plan
Ketamine therapy is one component of a broader treatment strategy. It is not a standalone cure for migraine disease. Neurologists use the relief period to initiate other preventive therapies. Patients can engage in physical therapy or behavioral therapy with greater ease. The treatment creates an opportunity to break the cycle of chronic pain. This allows for the establishment of more effective long-term management. Success depends on this integrated, multidisciplinary approach.
Ketamine infusion therapy represents a shift in the therapeutic landscape for severe migraine. It provides a scientifically grounded option for cases that defy conventional treatment. The therapy underscores the importance of specialized, neurological approaches to pain. Its role is specific, and its administration requires expert oversight. For eligible patients, it can offer substantial relief and a renewed capacity to engage with life. This treatment exemplifies progress in the pursuit of solutions for complex neurological disease. It brings a measure of hope to a challenging clinical reality.